On a sunny afternoon in March 2021, 18-year-old Adriana Metallides realized that her brother, 22-year-old Nick, hadn’t come out of his room all day.

With her mother watching through the FaceTime app on an iPhone, she pressed open his door to find him unresponsive, a water bong still in his hand.
Gwen Metallides raced home from her job as a surgical technologist at UPMC Mercy in Pittsburgh. On the two-and-a-half-hour drive to Marietta, Ohio, she learned her son was dead.
Synthetic opioids, primarily fentanyl, have driven up overdose deaths in the U.S. six-fold since 2015.
That’s the year fentanyl began appearing in street drugs in Allegheny County, said Alice Bell, overdose prevention coordinator for Prevention Point Pittsburgh. Two years prior, in 2013, just 3% of overdose deaths in the county involved fentanyl, according to the county’s overdose dashboard. Preliminary data for 2022 shows that number has shot up to 86%.
Nick Metallides, who grew up in Western Pennsylvania, had been dealing with chronic pain for years. He died from a fentanyl overdose.
Fentanyl didn’t become a household word until a few years ago, as the cheap, powerful drug used in hospital settings for anesthesia and pain control began to dominate the illicit drug market, once led by substances such as heroin. The widespread prescribing of pain medication helped to expand the market.

Now the discussion among many treatment experts, lawmakers and families has turned to harm reduction, which takes a holistic approach and considers a person's lived experience and the social structures that lead to drug use, such as poverty and trauma. Harm reduction aims to mitigate overdoses and alleviate the painful cycle of addiction by arming drug users with tools, such as fentanyl test strips, the overdose-reversing medication naloxone, and Suboxone and methadone to help prevent withdrawal and relapse.
Supervised consumption sites — which are not legal federally — have gained traction in a handful of states, including Rhode Island and New York. Proponents of such sites have advocated for decriminalizing drug use — a tenet of harm reduction — and recognize the reality that drug use occurs. Detractors argue the centers promote that very drug use.

And while Pittsburgh’s new Second Avenue Commons, which opened Downtown late last year, is not a supervised consumption site, it aims to address unmet needs of those experiencing homelessness, such as medical care and referrals to outside resources. It also offers “amnesty lockers” that visitors can use to store drugs and alcohol.
The challenge, harm reduction advocates argue, is reaching people where they are and helping those in need tap into resources when drug use is still largely seen as a character flaw.
“For most people, it takes six to seven attempts until sobriety sticks,” said Dr. Todd Wahrenberger, chief medical officer at Pittsburgh Mercy and a physician.

Nationwide, 2021 saw 107,000 overdose deaths — with nearly 66% involving fentanyl, according to the Centers for Disease Control and Prevention and the National Institute on Drug Abuse. The epidemic has a tight grip on Pennsylvania, which ranked eighth highest for total overdose deaths that year, and is ravaging Allegheny County’s communities too.

“There is no substance you can seek to purchase where there isn’t a significant likelihood that it will have fentanyl,” said Dan Palka, administrative director of R.O.O.T.S. (or Reaching Out On The Street), which provides trauma-informed care to people experiencing homelessness and is part of AHN’s Center for Inclusion Health.
Increased fentanyl use is tied, in part, to the rise of prescription opioids within the regulated drug supply. The CDC said prescription opioids led to 263,000 U.S. deaths from 1999 to 2020.
As regulations tightened in the 2010s, the illicit opioid market grew.
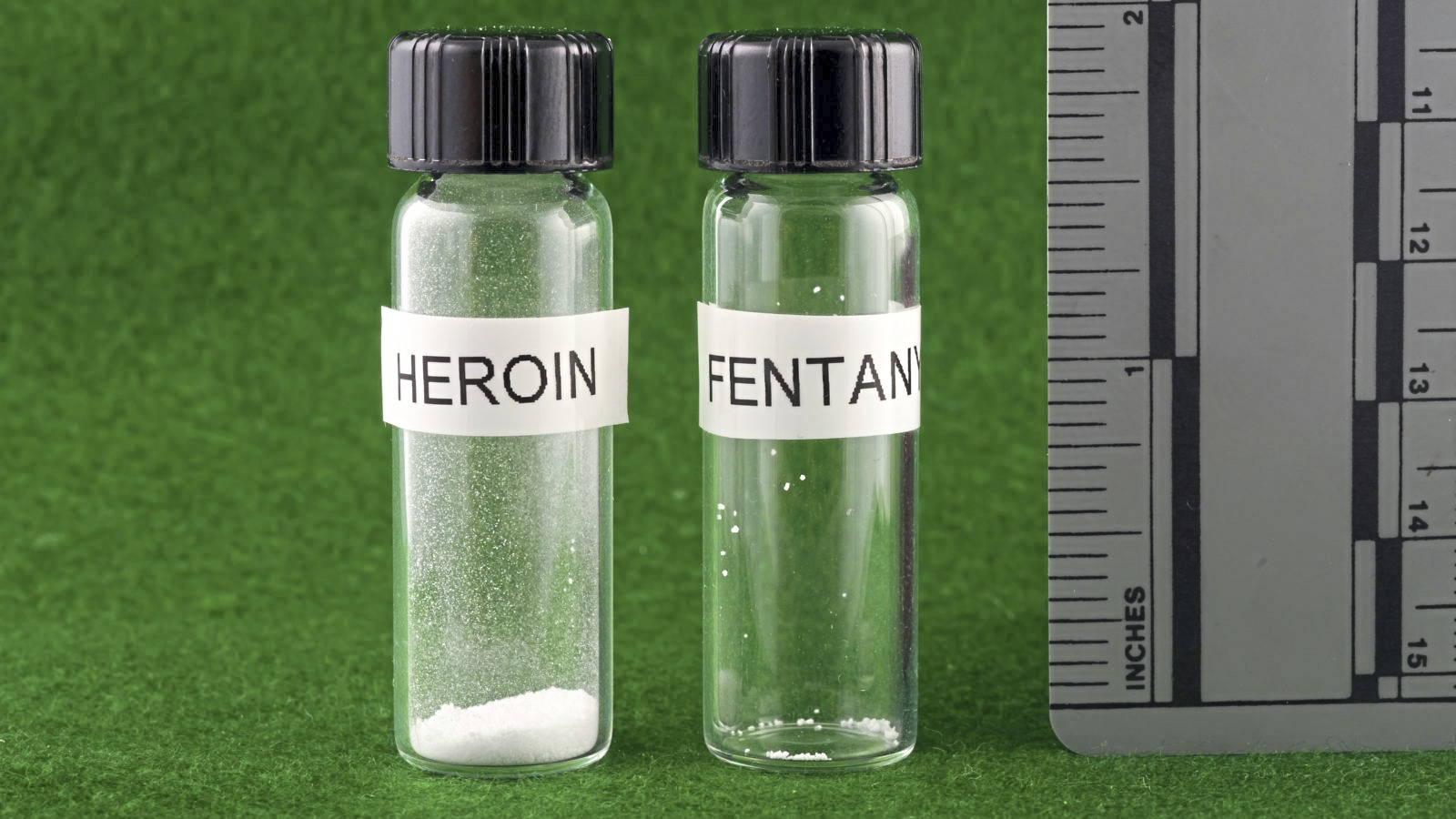
“Fentanyl is approximately 50 times more potent than heroin and 100 times more potent than morphine, with doses selling for the price of a six pack of beer,” Josh Shapiro noted in a report last spring. At the time, he was Pennsylvania attorney general; he was elected governor last November.
Fentanyl has also found its way into cocaine. In 2022, that combination made up 56% of fentanyl-related overdose deaths in Allegheny County, compared to 20% for fentanyl and heroin, said Otis Pitts, deputy director of Allegheny County’s Bureau of Food Safety, Housing & Policy, which oversees opioid-related policies.
“This is one of the reasons why fentanyl is killing people,” Ms. Bell said. Buyers don’t know whether something purchased on the street contains only a little fentanyl or a lethal dose.
“I can promise you that if you buy Xanax off the street, I can tell you what won’t be in it — Xanax,” said Dave Lettrich, the executive director of Bridge Outreach, a nonprofit in Pittsburgh that administers harm reduction and connects people to recovery services.

Gwen Metallides described her son as tall, with a shock of brown hair and a great sense of humor. He loved animals and kids, and he wanted to have a family someday — one like his own tight-knit family, which often held game nights.
Around age 17, he was treated at UPMC Children’s Hospital of Pittsburgh for a condition called a venous malformation, which caused pain and swelling in his legs. Nick underwent seven surgeries and had been prescribed OxyContin, his mother said.
Eventually, she said, he took to the streets to find ways to handle his chronic pain. He started smoking heroin and taking illicit Xanax.
Nick would have been a perfect candidate for harm reduction efforts. But as far as anyone can tell, he was never offered the chance.
Nick died from a combination of heroin, fentanyl and fentanyl analogs acetylfentanyl and fluorofentanyl, according to autopsy and toxicology reports reviewed by the Post-Gazette.

A UPMC spokesperson said Nick was cared for by several UPMC Children’s services and that “standard of care practices” were followed. He was discharged from treatment in May 2019.
“We understand the family of Nicholas Metallides is dealing with a tragic loss,” said the spokesperson. “The clinical care team here at UPMC Children’s has reached out to offer assistance to the family.”
Gwen said someone did call and ask whether the hospital could have done anything differently.
She didn’t work for a year following her son’s death; the burden of grief, she said, sapped her energy.
“I think about him every day,” she said. “It’s been really lonely.”

In November, the use of fentanyl test strips became legal in Pennsylvania. The strips can tell a user whether a substance contains the synthetic opioid.
Prevention Point now gives out the test strips, and, while Ms. Bell said their legalization was great news, she also said many people don’t use them because of how widespread fentanyl already is.
“We needed those [test strips] like five years ago, when it was still possible to find drugs without fentanyl in them,” Mr. Palka of R.O.O.T.S. added.
Dr. Anita Leon-Jhong, a UPMC physician and the co-medical director for Second Avenue Commons, said the test strips have alerted people to fentanyl in stimulants such as cocaine. “This is the population we’re pushing to use the test strips,” she said.
Another tool used to reduce overdose deaths is the readily available Narcan. Generically known as naloxone, the drug can reverse an opioid overdose by blocking spots in the brain where opioids dock. Not only does Narcan work, it is plentiful.
Narcan may be available over-the-counter at pharmacies soon. The FDA is expected to rule on March 29. It can currently be found at:

Prevention Point gives it out free at all five of its locations. R.O.O.T.S. also gives out Narcan, as do other centers within Allegheny Health Network, like the Center for Recovery Medicine, and pharmacies like Rite Aid and Hilltop.
The Allegheny County Jail distributes it to people upon release, and many Pittsburgh police officers carry it. NextDistro is a mailing service where anyone can sign up to receive free Narcan after completing short training online.
Soon, it could be even easier to obtain naloxone, commonly delivered as a nasal spray: In mid-February, an FDA panel unanimously voted to recommend naloxone be sold over the counter.
Suboxone, a combination of the opioid buprenorphine and naloxone, is an option for treating opioid addiction. Suboxone partially activates the brain’s opioid receptors, so it can help prevent cravings without being as addictive or dangerous as other opioids like heroin and fentanyl.
“They’re the most effective method we have” for opioid addiction treatment, Dr. Nora Volkow, director of the National Institute on Drug Abuse and a psychiatrist, said of Suboxone and the long-prescribed methadone, which helps people reduce or quit their use of heroin and other opiates. “The problem is they’re not … as widely available as they should be.”
Various programs such as AHN’s Center for Inclusion Health, UPMC Addiction Medicine Services and the county jail prescribe Suboxone and methadone, but people trying to access medication-assisted treatment in jail must have a pre-existing prescription.

Born in McKees Rocks, Mike Boylan started using drugs while at Sto-Rox Junior-Senior High School, mixing alcohol and Quaaludes, a hypnotic sedative. He was a star basketball player, and later enrolled in the Air Force, enduring “a brutal boot camp” in which he said he was injured. He sought out alternative sources for pain relief.
“I was a full-blown alcoholic and addict after that,” he said.
He came back to Pittsburgh and worked in fast-paced restaurant kitchens. His drug use continued; he started using cocaine, heroin, cannabis, crack cocaine and prescription painkillers. He had children; he started a furniture company in Kittanning.
While running his furniture store, he directed U-Hauls into the alleyway, exchanging inventory for quick cash for drugs. He lost the company in eight months.
“Your world shrinks to almost nothing when you’re using,” said Mr. Boylan, now 18 years sober and a certified peer specialist with Pittsburgh Mercy. “You do things, say things, and act differently than you ever would.”
There were times in 2004 when he spent $1,000 a day on drugs. “I had a very expensive habit,” he said. “And I lost everything.”
Experts who support the assessment that addiction is a disease agree that individual choice and control take a backseat when the brain activates craving, impulsivity and withdrawal pathways on an endless loop.
“If we’ve never had that experience, we think, ‘That person should be able to stop,’” said Dr. Volkow. “We are seeing it from our own experience.”
When a person uses a drug such as an opioid, the brain quickly adjusts to its new reality. Fentanyl activates opioid receptors, docking at sites that exist to process chemicals like endorphins. Studies have shown that when fentanyl activates these receptors, dopamine increases, flooding the brain to create a sense of euphoria.
The brain’s goal is always to maintain equilibrium, or homeostasis. For example, consider body temperature: Mild fluctuations outside of normal are felt right away as the body breaks out in fever or plunges into hypothermia.
With the brain now bathed in euphoria-inducing chemicals, it works to counteract and return to stasis. This neural boomerang drives cravings and is one reason withdrawal can be so agonizing.
People who use opioids regularly are no longer experiencing that fuzzy, ecstatic dose of pleasure. They are staving off withdrawal.
“The drive to escape harm is a good model for why people seek out their drug of choice to avoid withdrawal,” said Dr. Benedict Alter, an anesthesiologist in the Division of Pain Management at UPMC St. Margaret.
Mr. Boylan described withdrawal as 100 times worse than having the flu — body aches head-to-toe, cold sweats, diarrhea, a lack of appetite. “It could be Thanksgiving dinner and your family's waiting for you. And if you don't have any [drugs], you can't do it. You won't make it,” he said.
Because fentanyl is so potent, withdrawal can occur just two to three hours after taking the drug in those who use regularly. By comparison, for heroin, it can take eight to 10 hours.
Someone who used pure heroin could work a full shift at a job before withdrawal set in. With fentanyl’s shorter cycle, life is more complicated, further trapping users in a loop they can’t escape.
Even after a month without opioids, a person can still feel the effects of withdrawal, said Mr. Boylan. “You need 60 days, at least, even to feel physically better.” He recommended a minimum of six months in recovery. He spent two years at the last recovery center he attended for treatment.

An emerging treatment option in the U.S., called supervised consumption, allows people to use drugs inside a specific facility, usually in an injection booth with medical professionals on stand-by.
Also known as safe-injection sites, they are not without controversy. Detractors argue that such facilities encourage drug use. Advocates point to the inevitability of drug use, and the dangerous potency of fentanyl.
Other countries, including Canada, have a longer history with safe-use sites.
Rhode Island was the first state to authorize supervised consumption in July 2021; later that year, two centers opened in New York City. Supervised consumption is still illegal under federal law.
In Philadelphia, the nonprofit Safehouse has been embroiled in a lawsuit with the U.S. Department of Justice as it seeks to become a supervised consumption site. Safehouse, which dates to late 2018, has encountered legal challenges since its inception.
Insite, a supervised consumption site in Vancouver, B.C., opened in 2003 on Hastings Avenue, a street known for high rates of drug use and homelessness, but also celebrated for its proximity to many music venues. Insite recorded more than 170,000 visits in 2019, according to its website, and its team intervened in 1,314 overdoses that year.
No deaths have occurred at Insite during its 20 years in operation. But in 2019, when more than 1,000 people were saved at the site, opioids or stimulants were linked to 1,017 deaths on British Columbia’s streets.

Pittsburgh’s Second Avenue Commons has been lauded for its “amnesty lockers” that visitors can use to store drugs or alcohol. But Mr. Palka worries if fentanyl withdrawal occurs in two to three hours, people might need to leave the shelter to suppress creeping withdrawal.
Various sources involved in Second Avenue Commons’ planning said there were conversations about it being a supervised consumption site, but the idea was rejected due to logistical issues and a general discomfort.
“From a harm reduction standpoint, it makes sense; it’s just legally complicated,” said Dr. Leon-Jhong. “There has been community backlash to the idea.”
“Most experts absolutely support supervised consumption,” said Mr. Lettrich, of Bridge Outreach. “But most people in power tend to make decisions based on community consensus instead of expert opinion. That’s the challenge.”

Mayor Ed Gainey has expressed interest in harm reduction services including syringe exchanges, but he did not respond to repeated requests for comment regarding supervised consumption in Pittsburgh. His administration also did not respond to multiple interview requests.
Jennifer Smith, the secretary of Pennsylvania’s Department of Drug and Alcohol Programs, said efforts were being made statewide to bridge this gap, including garnering approval to operate supervised consumption sites.
“There has absolutely been some benefit shown by other countries who have adopted these models in terms of wound care,” said Ms. Smith in a Dec. 16 virtual town hall meeting about combating the opioid crisis. Injecting drugs can put a person at risk for infection; staff on-hand can help treat that complication. “There’s a lot to share and investigate in this space, and it certainly will take a joint effort.”
Madeleine Dean, a Democratic congresswoman from suburban Philadelphia, also participated in the December town hall meeting and has advocated on Capitol Hill for funding to expand harm reduction services.
“This is part of an evolution,” she said. “We have to push forward in terms of education and disband the myth that we are encouraging drug abuse” with harm reduction tools like safe-use sites, syringe service programs and Narcan training.

Because many who use drugs end up unhoused, the stigma around drug use mounts higher, as judgments — addict, junkie, criminal — pile on.
“None of them want to be in the position that they are,” said Marianne Sinisi, of Altoona, who lost her son Shawn to a fentanyl overdose in 2018. “I do know that [drug users] are not thinking clearly. The drug is.”
The cycle is perpetuated by community exile and a lack of resources to ease reintegration. “They can’t keep coming back out and having hatred spewed at them, because how do they get well?” said Ms. Sinisi.
Since her son’s death, she has fought for harm reduction and compassionate care of people who use drugs, starting a nonprofit called Families United for Change, which tackles drug addiction stigma and fights for related legislation.

“If your child is a ninth grader and they get leukemia, they’ll organize a 5K for you. But if you have a 10th grader doing heroin, you don’t tell anyone. You cover it up,” said Dr. Wahrenberger, of Pittsburgh Mercy.
Dr. Wahrenberger would like to see the Pittsburgh community explore more options in harm reduction, especially since other countries, like Switzerland, have seen success with a regulated drug market.
“We’re losing the war,” he said. “There’s evidence-based treatment out there we’re not using because we still see this as a character flaw issue.”
Someone in recovery has the highest likelihood of relapsing and dying from an overdose in the first month they leave a program, said Dr. Wahrenberger. Accessible resources, such as stable housing and medication-assisted treatment, can make a difference.
Shawn Sinisi had nieces and nephews he loved dearly, but found it difficult to spend real time with them while stuck in the revolving door of prison and drug court. His story was outlined in a recent podcast, “The Mayor of Maple Avenue.”
“I could see the pain in his eyes when his niece and nephew wouldn’t say goodbye to him,” said Marianne Sinisi. “It broke my heart.”
“So many people are dying from this,” she went on, “that if this was a war, we'd be talking about it every day.”
Hanna Webster: hwebster@post-gazette.com
Correction: An earlier version of this story had the incorrect year for when Mike Boylan spent $1,000 a day on drugs. It was 2004.
Hanna Webster
James Hilston
Ed Yozwick
Laura Malt Schneiderman
Advertisement
Advertisement