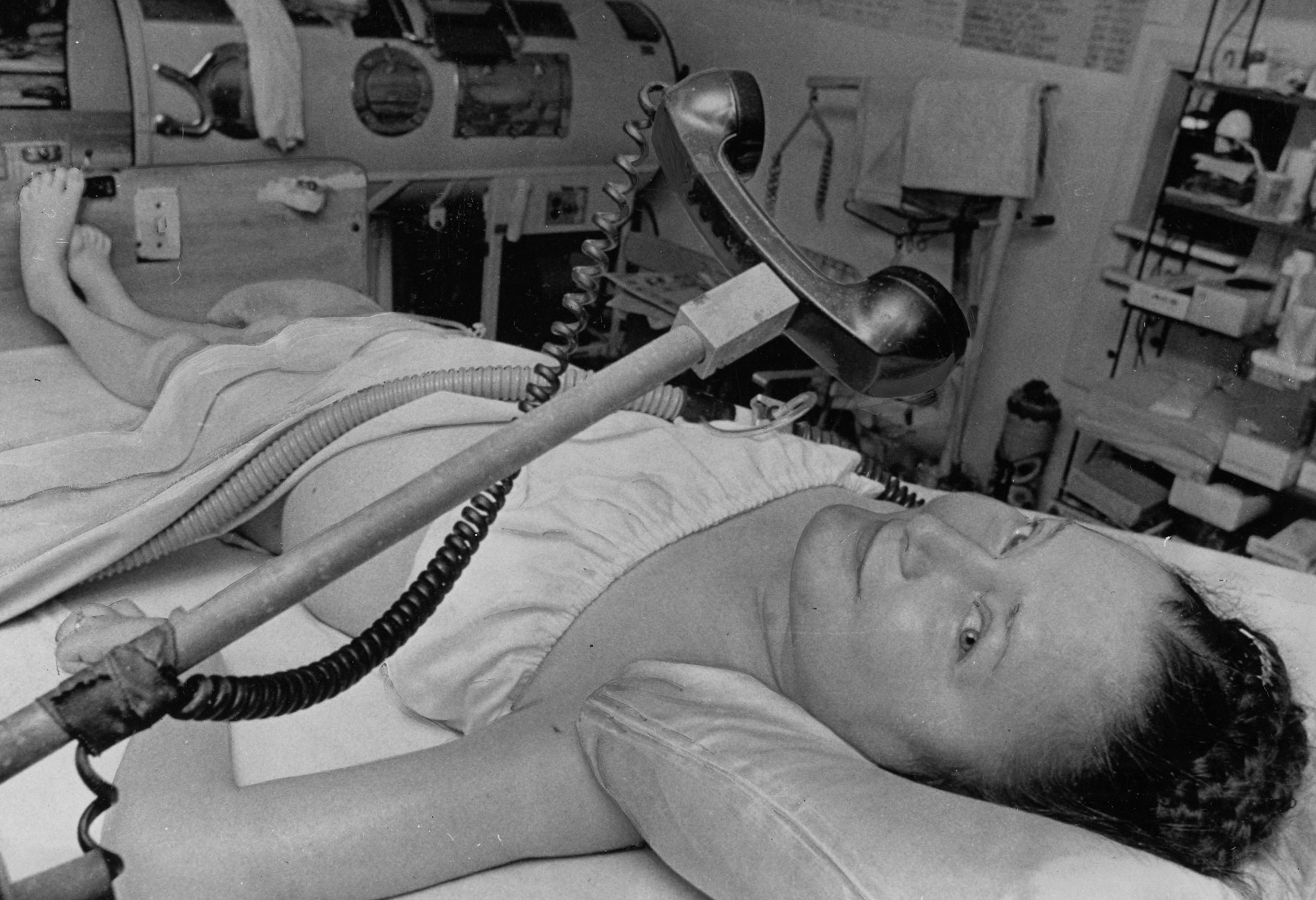
Polio paralyzed Bettye Erickson in 1946. In this 1976 photo, she is being put into an iron lung for the night. During the day, she relied on a breathing assistance machine. (UPI/Post-Gazette Archives)
Until that point, polio had been a deeply feared disease with no cure. Spread through contact with infected human waste and, occasionally, through contact with droplets from an infected person’s sneeze or cough, it had become many parents’ worst nightmare.

With news of a 10-year-old girl and her aunt, 17, being hospitalized for polio, Canonsburg health officials closed the borough public pool in July 1948. (Post-Gazette Archives)
The polio virus existed on a small scale for possibly thousands of years, but in 1900, epidemics broke out in the U.S. and Europe. Experts believe that before then, mothers who survived the virus passed some immunity to their children in the womb or through breastfeeding, according to “Polio: A 20th Century Epidemic,” a 2018 article from London’s Science Museum.
Better sanitation in the 20th century meant fewer people were exposed to polio in their early years and fewer built up immunity. Women were less likely to give immunity to their babies. Ironically, better sanitation led to higher incidence of the disease.
After 1916, the disease began a cycle of surging every summer in the U.S., with the most serious attacks coming in the 1940s and 1950s. In 1952, the U.S. reported 57,879 cases and 3,145 deaths, according to a 2017 article by Sophie Ochmann and Max Roser published on Our World in Data.
Some swimming pools, such as the one in Canonsburg, were closed as a precaution, according to a July 28, 1948, article in the Pittsburgh Sun-Telegraph.
About 4% of people exposed to the virus suffered fever, sore throat, headache, vomiting, fatigue, back pain or stiffness, pain or stiffness in the arms or legs and muscle weakness or tenderness. A small percentage experienced more severe symptoms.

In a rare photograph showing President Franklin D. Roosevelt in his wheelchair, the president poses in February 1941 on the porch at Top Cottage in Hyde Park, N.Y., with Ruthie Bie, the granddaughter of the caretaker of the cottage, and his dog, Fala. (Franklin D. Roosevelt Presidential Library & Museum)
Within a week, the sufferer suddenly had no reflexes, the muscles ached severely and limbs were loose or floppy.
In extreme cases, extremities, usually the legs, became paralyzed temporarily or permanently. The patient had to rely on leg braces or wheelchairs. In permanent cases, legs could atrophy and feet could become deformed. Temporary paralysis could last a year. According to the World Health Organization, about 1 in 200 polio infections leads to permanent paralysis.
In up to 10% of permanent paralysis cases, the disease destroys the ability to swallow or breathe, leading to death if the patient receives no automated assistance. The first machine to help patients breathe was called an iron lung.
Franklin D. Roosevelt, U.S. president from 1932 to 1945, famously contracted polio at age 39 and lost the use of his legs. For public appearances, he used a cane and heavy leg braces and leaned on a son or adviser for balance as he swung his legs forward, making it appear as if they worked.
Other well-known polio survivors include KDKA-TV news anchor Stacy Smith; retired professional golfer Jack Nicklaus, who believes his sore joints might signal post-polio syndrome; film director Francis Ford Coppola; singers Judy Collins and Joni Mitchell; and actors Alan Alda and Donald Sutherland. All of them as children spent lonely weeks or months in bed recovering.