Economics of spinal fusion: Back surgery complicated, expensive and increasing
By Rich Lord Pittsburgh Post-Gazette
The number of Pennsylvanians having spinal fusion surgery for back pain recently surpassed 20,000 a year, and concern over the procedure is rising from several fronts: a state agency that monitors health care, former doctors who filed a whistleblower lawsuit and some patients whose surgeries did not go well.
In 2014, 21,393 Pennsylvania adults underwent spinal fusions, up from 12,794 in 2004, according to a state study released in June. The frequency of fusions doubled for residents 65 and older.
For most, the surgery, aimed at easing back pain, goes off without complications.
But fusions are expensive, complicated and can go wrong. For the one-in-seven Pennsylvania fusions that were covered by Medicare, the government paid an average of around $24,000.
The state-funded Pennsylvania Health Care Cost Containment Council reported in June that 3.3 percent of fusion patients had complications while in the hospital, and 5.4 percent were readmitted for unplanned reasons.
Even as the number of back operations increases, benefits are elusive for many people, according to a 2011 British Medical Journal study, which summarized four studies that found rehabilitation worked about as well as surgery for pain and disability.
Spinal fusions by year
Spinal fusions in Pa., 2004 to 2014
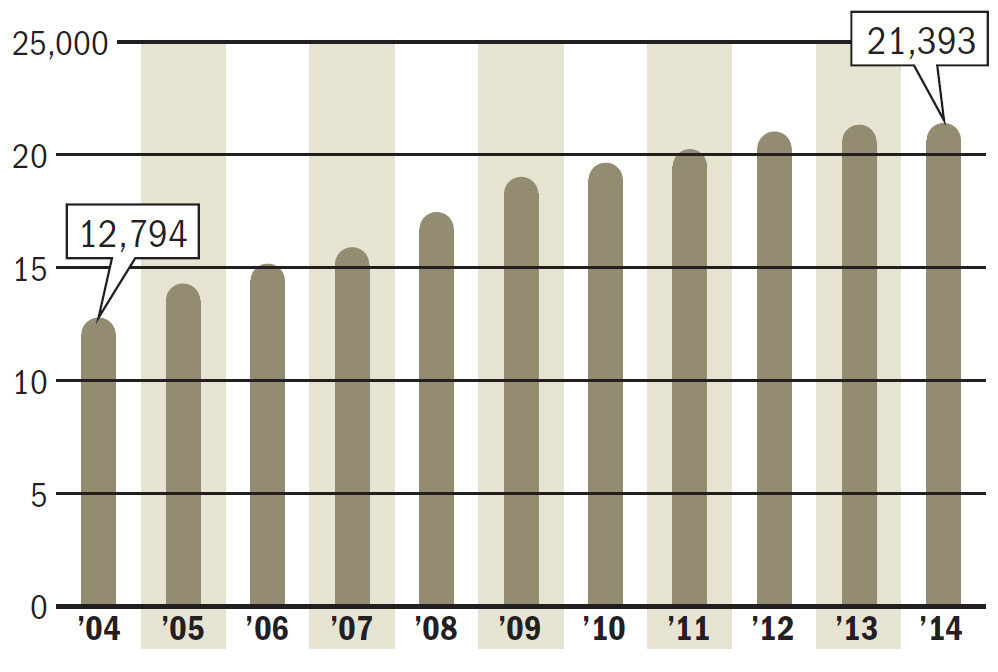
Source: Pa. Health Care Cost Containment Council
So why are fusions increasingly prevalent?
“Almost everybody, by X-ray, has a bulging disc” and back-pain-prone seniors “all have health insurance because they’re all covered by Medicare,” said David B. Nash, dean of the Jefferson College of Population Health, at Thomas Jefferson University in Philadelphia.
A whistleblower lawsuit filed by three former UPMC employees and unsealed in July charges that the back surgery boom is fueled by another element: money. The lawsuit zooms in on a national trend in which most neurosurgeons and orthopedists now sign contracts with hospitals that pay them bonuses if they exceed a base number of surgeries.
“What if more people would ask, ‘Doctor, do you get paid more if you do this operation than if you didn't?’ ” said neurosurgeon Matthew Quigley, who left the Allegheny Health Network in Pittsburgh in 2014 after nearly three decades. He said hospital administrators had asked him to sign a contract that would tie his pay to the number of procedures he performed. “I think it would be very sobering after a while.”
“If I’m going to get paid each time I do it, I’m going to do as many as I can,” said Michael Cassidy, a Downtown attorney with Tucker Arensberg who negotiates contracts for doctors and notes such incentives are legal.
A 2014 analysis of low-back surgeries from 2001 through 2011 by the Dartmouth Institute for Health & Clinical Practice found that compared to the national average, Pittsburgh-area Medicare beneficiaries were 44 percent more likely to undergo lumbar fusions. (Also above the national average were the Altoona, Danville, Harrisburg, Johnstown, Lancaster and York areas, while Allentown, Erie, Philadelphia, Reading, Sayre, Scranton and Wilkes-Barre were below.)
The Pennsylvania Health Care Cost Containment Council also found that the number of fusions conducted per resident in 2014 was higher in Western Pennsylvania than in the central or southeastern regions of the state.
That could, in part, reflect people traveling from outside the region to avail themselves of experienced surgeons at Pittsburgh hospitals.
Rate of spinal fusions more than doubles in 10 years
The population-based rates of spinal fusion for Pa. for ages 45-64 and 65 and older
Ages 45-64 Ages 65 and older
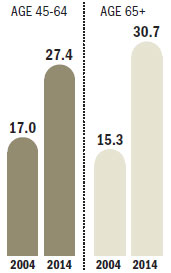
Source: Pa. Health Care Cost Containment Council
UPMC Presbyterian was the fusion capital of the state in 2014, logging 2,350 such surgeries. The health system billed around $323 million for the surgeries, for which it doubtless received a lower amount based on varied insurance reimbursement rates.
In Allegheny County in 2014, UPMC Passavant ranked second among hospitals for fusions, at 618, while 561 of the surgeries were done at third-place Allegheny General Hospital. That year, UPMC hospitals conducted 4,508 spinal fusions, versus 1,495 for the Allegheny Health Network, according to the health care council.
The council doesn’t know why fusions are so common in Western Pennsylvania, said Joseph Martin, its executive director, but his board is concerned with “these dramatic increases [in back surgeries], the impact that it has on costs, the impact that it has on lost productivity.”
“It’s really hard to definitively say, ‘Was this back surgery appropriate or inappropriate?’ And how much of the increase in back surgery was [unnecessary]?” said Harold Miller, president and CEO of the Downtown-based Center for Healthcare Quality and Payment Reform.
“However, when you see it go up that much, you can’t help but say, ‘Hmm.’ ”
A review of pending medical malpractice lawsuits filed against Pittsburgh-area neurosurgeons identified one back operation the patient said was “completely unnecessary” and another that alleged the surgery was not justified by the patient's medical history or condition. Other lawsuits were filed by patients who allege that their complications stemmed from a less invasive but more complex operation that pays the surgeon as much as three times more than simpler back surgeries, but with sometimes fatal consequences.
The federal government is forcing many hospitals and physicians to accept new payment methods, aiming to reward “value, not volume,” for knee and hip surgeries. Such a shift could encourage cheaper treatments, like physical therapy. With coming Republican control of the federal government, it’s unclear whether that model will spread.
Until then, in a world full of aching backs, it’s no surprise that surgeons readily operate. “When you have a hammer,” said Dr. Nash, “everything looks like a nail.”
Spinal fusions by hospital
Southwestern Pa. hospitals that performed more than 100 spinal fusions in 2014
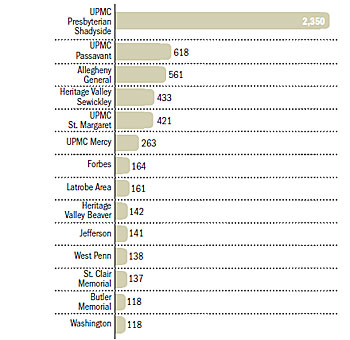
Source: Pa. Health Care Cost Containment Council
The whistleblower lawsuit
In 2012, three former UPMC employees — neurosurgeon J. William Bookwalter, neurologist Robert J. Sclabassi and surgical technician Anna Mitina — filed suit against UPMC under seal, alleging that the Pittsburgh health-care giant systematically overbilled the government by giving doctors too much incentive to conduct surgery.
They cited the False Claims Act, in which a person who sees fraud against the federal government can sue on the government’s behalf. The Department of Justice can let the whistleblower pursue the case independently, or lend its legal muscle. The whistleblowers and their attorneys can get anywhere from 15 percent to 30 percent of any eventual settlement or judgment. The government gets the rest.
UPMC in July agreed with the Justice Department to settle parts of the lawsuit for $2.5 million, while denying any wrongdoing. The settlement involved allegations that certain neurosurgeons submitted false claims for assisting with or supervising surgical procedures performed by other surgeons, residents, fellows or physician assistants, when those neurosurgeons did not participate to the degree required. Another claim involved a neurosurgeon submitting claims to Medicare for levels of spinal surgery not actually done.
The whistleblowers are continuing to pursue other claims about how UPMC pays its doctors. In an October motion to dismiss the rest of the lawsuit, UPMC characterized its arrangements with doctors as nothing more than an “effort-based incentive compensation system” and noted that a “productivity bonus based on services performed personally by the physician” is specifically allowed under federal law.
The lawsuit alleges that in 2006, Amin Kassam became chairman of its department of neurological surgery, and “embarked upon a campaign to increase the volume of surgical procedures.”
Dr. Kassam did not respond to an interview request, and his current employer, Aurora Health Care of Milwaukee, did not make him available.
Who pays for spinal fusion surgeries in Pa.?
Percent of spinal fusions covered in Pa., 2014
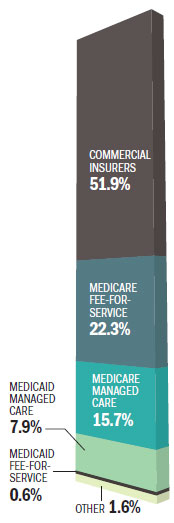
Source: Pa. Health Care Cost Containment Council
Doctors' work volume is measured in “work relative value units,” or wRVUs. The federal government might assign a value of a few dozen units to a simple surgery, or more than 70 for a complex procedure. Medicare reimbursements to the doctor are then based on the unit number, modified for the geographic location in which the surgery is conducted.
Payments by other programs and insurers for similar treatments are often based on, but higher than, the Medicare reimbursements.
During the chairmanship of Dr. Kassam, who earned $1.46 million in the 2007-08 fiscal year and left UPMC in 2009, each neurosurgeon was “required to generate a minimum number of wRVUs per calendar year in order to earn his or her base compensation,” according to the ex-employees’ lawsuit.
The ex-employees, represented by attorney Andrew Stone, allege that while a “busy clinical and surgical practice” translates to 15,000 work units in a year, some of UPMC’s neurosurgeons reached multiple times that level.
High production earned the doctor “incentive compensation or ‘bonus pay’ for each wRVU generated above the physician's annual base wRVU number at the rate of $45 for each additional unit, according to the lawsuit.
The lawsuit suggests that $45 per unit can only be interpreted as an “illegal kickback” to the physician by the hospital — which earns several times as much as the doctor for facility fees and services related to the surgery.
A UPMC spokeswoman declined to address questions presented for this story. In its motion to dismiss the lawsuit, the health-care system called the work units “a standard measure commonly used ... to measure and reward productivity” and said paying doctors on that basis is “not only lawful but common practice.” And it wrote that the ex-employees failed to specify “even a single unnecessary surgery.”
Feeling the pressure
Mr. Cassidy, the attorney who represents doctors in contract negotiations, said pay-for-volume contracts started around 20 years ago and are now “almost universal,” and that paying doctors more for units than Medicare pays is sometimes appropriate. “It’s done routinely for stars,” he said, as a means to attract and retain top talent.
A lot of hospitals draw a line, saying they won’t pay bonuses for additional units that put a physician in the top 10 percent of producers for his or her specialty nationally. Some argue that a bonus that pushes doctors to reach the upper echelons of production could be construed as violating the law.
“Hospitals always say, ‘We’d love to do that, but it’s illegal,’ ” Mr. Cassidy said. “And the reaction is, ‘No, it’s not.’ ”
Many academic medical centers used to pay straight salaries, “so there was more of a separation between exactly what a surgeon, for example, does and what he or she gets paid,” said Peter Angelos, a surgeon and associate director of the MacLean Center for Clinical Medical Ethics, at the University of Chicago. Most, though, “have shifted to making the compensation for a physician much more driven by RVU production,” he said.
Doctors, he said, now have to ask themselves: “Is in fact the recommendation based on the patient needing the procedure, or is the recommendation made based on the fact that I can bill for it, I can generate RVUs for it?
“I feel that pressure of, ‘OK, if I do more operating, then I do more RVUs.’ I feel that pressure more than I did 10 years ago,” he said. He added that doctors concerned with their reputations “should be making decisions based on our patient’s best interest.”
Paying for outcomes
Since April, many knee and hip surgeries have been covered under a different formula.
In 67 metropolitan areas, including Pittsburgh, health-care providers billing Medicare for hip and knee replacement surgery now receive a bundled payment, which covers everything from the initial hospitalization through the patient’s recovery.
In theory, said Mr. Miller, providers “get a predetermined amount based on the patient needs, not based on what you did for them.” He has criticized the formulas used, saying they may not adequately pay for the toughest cases.
Keith Kanel, chief medical officer of the Pittsburgh Regional Health Initiative, noted that today, if a surgeon must conduct a spinal fusion twice because of complications, the government pays twice. The bundled payment system could change that.
The initiative — funded by foundations and the state, and led by a board that includes public officials and executives from both major health and insurance systems — pushes for zero complications and has helped hospitals to achieve that for some procedures.
“When the systems are given fixed payments, and have to take care of the complications out of their own pocket, it forces them to double down” on quality, Dr. Kanel said.
Allegheny Health Network has been adding quality of care and outcomes metrics to physician compensation contracts, said Tony Farah, a cardiologist and chief medical officer at the region’s second largest hospital system. But the transition to pay based on “outcomes rather than volume” won’t be instantaneous, he said.
“You can't flip a switch because no one is ready,” he said.
AHN plans to hold physician meetings to solicit input on how doctors should be paid, getting buy-in for the shift, he said. “We'll pull together committees of doctors and say, how would you get paid in the future?”
For now, volume-based compensation packages are the mainstay of physician contracts. Doctors, Dr. Angelos said, have to ask themselves, “Is in fact the recommendation based on the patient needing the procedure, or is the recommendation made based on the fact that I can bill for it?”
Part 2
Part 3

Mary Margaret, shown with her husband, Williard Rhodes, was left disabled by back surgery at UPMC Shadyside Hospital. Gracey Evans/Pittsburgh Post-Gazette
A patient's story: Lawsuit claims doctors' pay influences decisions
By Kris Mamula Pittsburgh Post-Gazette
At the end of a concrete driveway is a three-bedroom house and a motor home still draped with a tarp at the height of summer, a reminder of all Mary Margaret and Bill Rhodes have lost.
The couple retired within a year of each other a decade ago and had the house built in Jeannette. They planned to spend their remaining years together traveling and living near their grandchildren.
“We traveled. I used to drive,” said Mrs. Rhodes, whose back surgery for pain relief went awry at UPMC Presbyterian Hospital in 2013, leaving her mostly confined to a wheelchair. “Our life changed in an hour, seconds.”
She awoke from surgery Dec. 3, 2013, with a sharp pain in her upper back. Her surgeon, Peter Gerszten, told her the operation went “beautifully,” she said. The pain intensified and Mrs. Rhodes stayed overnight at the hospital instead of going home after a procedure that was supposed to be outpatient.
Mrs. Rhodes, 75, a retired executive secretary, was moved to a nursing home where the pain worsened until she was screaming in agony. She was taken to UPMC East Hospital in Monroeville by ambulance, then flown to UPMC Presbyterian by helicopter Dec. 7, 2013, for emergency back surgery.
Mrs. Rhodes can walk only a few steps at a time and her back pain is constant. Mr. Rhodes, 76, a retired real estate specialist at the Pennsylvania Liquor Control Board, is his wife’s primary caregiver.
The medical malpractice lawsuit that the Rhodeses filed against the surgeon and an earlier whistleblower lawsuit in federal court raises questions about the widespread practice of paying doctors based on volume — the number of medical procedures performed — which the lawsuits claim can wind up hurting patients.
The malpractice claim the Rhodeses filed in 2014 against UPMC alleges that the health system’s commission-based method for paying Dr. Gerszten tainted his judgment, causing him to recommend an operation that was “completely unnecessary and absolutely contraindicated,” according to case filings.
Pittsburgh-based UPMC has denied the claims, but the allegations mirror ones contained in a whistleblower lawsuit that was filed under seal in U.S. District Court by three former UPMC employees a year before Mrs. Rhodes met with Dr. Gerszten. UPMC has moved to dismiss that lawsuit, maintaining that the way it pays its doctors is legal and common throughout the health-care industry.
The federal lawsuit alleges that UPMC created a culture among its neurosurgeons that prized volume of medical procedures over the best interests of the patient.
UPMC administrators “openly encouraged and contractually incentivized physicians” to boost the number of procedures done “regardless of whether surgery is medically necessary for patients,” the lawsuit alleged.
UPMC spokesman Paul Wood said that Dr. Gerszten would not be available for comment.
What’s more, assessing back problems can be difficult, according to former Allegheny General Hospital neurosurgeon Matthew Quigley, who left Pittsburgh-based Allegheny Health Network in 2014 after administrators asked him to sign a contract that linked number of procedures performed to earnings.
“There’s no objective way to establish a benchmark for what constitutes a legitimate reason for a back operation,” he said. “It depends on the eye of the beholder and what their interests are.”
The Medicare managed care coverage that Mrs. Rhodes carried through UPMC Health Plan at first would not pay for the operation because such procedures were considered “extremely rare and should only be done in limited circumstances,” according to the Rhodes’ lawsuit, which was filed by medical malpractice lawyers Harry S. Cohen & Associates.
Dr. Gerszten’s office successfully appealed the insurer’s denial, according to the lawsuit. In court filings, Mr. Cohen said he intends to prove the link between commission-based compensation and Mrs. Rhodes’ surgery. A trial is scheduled for next year.
Part 1
Part 3

View a UPMC video of minimally invasive spinal fusion surgery.
Less invasive spine surgery: Small but significant risk of infection
By Kris Mamula Pittsburgh Post-Gazette
The operation planned for Gary Pettitt would cause less bleeding, ease his back pain and speed recovery when compared to traditional spine surgery, his doctor told him in 2008.
What the 45-year-old Tioga County man said he didn’t know is that his health insurer would pay the physician at least twice as much for the planned minimally invasive option as for traditional open disc repair.

Gary Pettitt and his wife, Norma, of Tioga County are dealing with the aftermath of his back surgery.
In a pending medical malpractice lawsuit that Mr. Pettitt and his wife Norma filed against UPMC and Peter Gerszten in 2010, Mr. Pettitt also said he was not told about a rare complication of the minimally invasive operation: a raging infection that nearly cost Mr. Pettitt his life and left him in chronic pain.
A UPMC spokeswoman said the system doesn’t comment on pending litigation.
“The doctor said I was going to work after the surgery,” said Mr. Pettitt, a truck driver, who is on disability. “Today, I can’t even sit to drive. Oh my God, it’s terrible.”
Mr. Pettitt’s lawyer, Clifford Rieders of Williamsport, Pa., subpoenaed Dr. Gerszten’s contract and information about his salary, benefits and bonuses, drawing a UPMC objection Oct. 31, saying the request had “no reasonable basis.” Trial is scheduled for early next year.
Back problems are among the most common medical complaints, with an estimated 10 million adults suffering from chronic back pain each year. The vast majority heal over time without surgery, but about a half million people undergo spine surgery for relief of persistent pain.
Traditional vs. minimally invasive
There are essentially two approaches to spinal fusion: traditional and minimally invasive.
Both kinds of surgery have about the same results after a year, experts say, but the newer, minimally invasive operation takes about half as long and pays doctors nearly twice as much as the traditional surgery. Patients prefer minimally invasive procedures because recovery can be faster than with open disc repair.
But minimally invasive back surgery also has a rare complication that traditional surgery does not: a punctured colon, which can be fatal.
Minimally invasive back surgery, where the surgeon uses a small incision in the buttock or flank to reach the spine, is more complex than conventional open back surgery — giving it a higher work unit value by Medicare. The number of work units determines how much doctors are paid for various medical procedures.
“These minimally invasive procedures are gimmicks,” said Nancy Epstein, a neurosurgeon at Winthrop University Hospital in Mineola, New York, who has studied the techniques. “The complications have been horrendous.”
Michael Steinmetz, co-director of Cleveland Clinic’s Center for Spine Health, said neither surgical approach is superior after a year. “Fusion results are unpredictable, which gives it a bad name,” Dr. Steinmetz said.
Minimally invasive back surgery also has another complication that Dr. Steinmetz said is underreported: thigh and leg weakness caused by nerve damage incurred during the operation, which can be permanent.
In light of such research, questions persist about the sharp run-up in the number of operations, which have been fueled by an aging population and advancements in spine surgery.
Vince Fink, a 67-year-old, self-employed home security technician from Hubbard, Ohio, said he turned to UPMC doctors for advice when he was having problems.
“I was flying blind,” said Mr. Fink, who filed a medical malpractice lawsuit against UPMC neurosurgeon Adam Kanter in 2014 over a minimally invasive spine surgery, claiming that it resulted in pain and an infection. “I was depending on their expertise to guide me.”
In the lawsuit, Mr. Fink said the procedure prompted numerous trips to hospital emergency rooms and two subsequent operations on his back. He lost 30 to 40 pounds during the ordeal at a time when his wife, a cancer survivor, was dealing with her own health issues, he said.
A UPMC spokeswoman said that Dr. Kanter was not available for comment.
Dr. Kanter was also named in a 2011 malpractice lawsuit filed by a Westmoreland County son and daughter whose 54-year-old mother, Diane Guidas, died four days after minimally invasive back surgery was done in 2009. The cause of death was a massive infection caused by perforation of the colon, the same complication Mr. Pettitt suffered.
Lawyers for the family declined to comment, and the case is scheduled for trial in March. A trial in the Allegheny County Court of Common Pleas is also scheduled for next year in a medical malpractice case filed against Dr. Kanter in 2012 by Alice and Barry Ferguson of Somerset County.
The Fergusons’ lawsuit claims that Dr. Kanter improperly placed a medical implant in Mr. Ferguson’s spine in July 2010 during minimally invasive back surgery, compressing the nerve and causing balance problems and numbness in his left knee. The operation was not warranted by Mr. Ferguson’s condition or medical history, according to the complaint.
A lawyer for the Fergusons declined to comment on the case, which is scheduled for trial in January.
A premium for certain procedures
Although doctors disagree on how well spinal fusion works, minimally invasive procedures take less time and pay doctors and hospitals more than conventional back surgery. Medicare assigns about 28 work units for the conventional approach to disc repair, but about 77 units for the more complex operation, such as the one Mr. Pettitt underwent.
Using Medicare’s reimbursement formula, the higher number of work units translates into $979.64 for the surgeon for conventional back surgery and $2,732.04 for the minimally invasive operation — a 178 percent premium, according to a surgical billing specialist.
The premium can balloon to 10 times the value of the simpler procedure, depending on scope of the operation, according to a whistleblower lawsuit filed by lawyer Andrew Stone, principal of the Downtown-based Stone Law Firm LLC, on behalf of former UPMC employees J. William Bookwalter, Robert Sclabassi and Anna Mitina.
Hospitals also benefit financially from the higher work units of their doctors, typically receiving four to six times the amount that surgeons are paid, billing experts say.
UPMC’s neurosurgeons are among the system’s highest paid employees, but could a surgeon’s judgment really be affected by volume-based compensation packages?
“That’s got to have an impact for some people,” Cleveland Clinic’s Dr. Steinmetz said. “But I’d like to think that all of my colleagues wouldn’t be impacted by it.”
Unlike most hospitals in the country, Cleveland Clinic pays its doctors a flat salary, regardless of the number of procedures they do. “Salary doesn’t push us to do anything,” he said.
Part 1
Part 2