
COVID-19 has claimed the lives of at least 82 residents of the Brighton Rehabilitation and Wellness Center since March.
Families of the victims, plus medical professionals and state and federal investigators, all are asking why.
The Pittsburgh Post-Gazette set out to answer their questions. It found during a five-month investigation that actions the Beaver County nursing home owners and managers took in the years before the onset of COVID-19 likely contributed to the virus’ spread there. And once Brighton officials knew there was an outbreak, they were slow to respond and failed to properly train the home’s staff in even basic infection-prevention protocols, the Post-Gazette investigation found.
What ensued was one of the deadliest COVID-19 outbreaks of any nursing home in America.

The last time Keri Boyer visited her father at Brighton Rehabilitation and Wellness Center, on March 7, three weeks before he died of COVID-19 and five days before a global pandemic would be declared, she noticed little had changed at the nursing home.
No one was wearing masks or gowns. There was no screening of visitors or staff. The typically overwhelmed nursing assistants scrambled to care for the more than 50 residents — most of them packed four to a room — in her father’s dementia unit on the 4th floor of the East wing of the massive building.
By the time the virus finished raging through Brighton in June, her 73-year-old father, Earl Denbow Jr., and at least 81 other residents had died in what became one of the worst nursing home death tolls in Pennsylvania and among the deadliest nationwide.
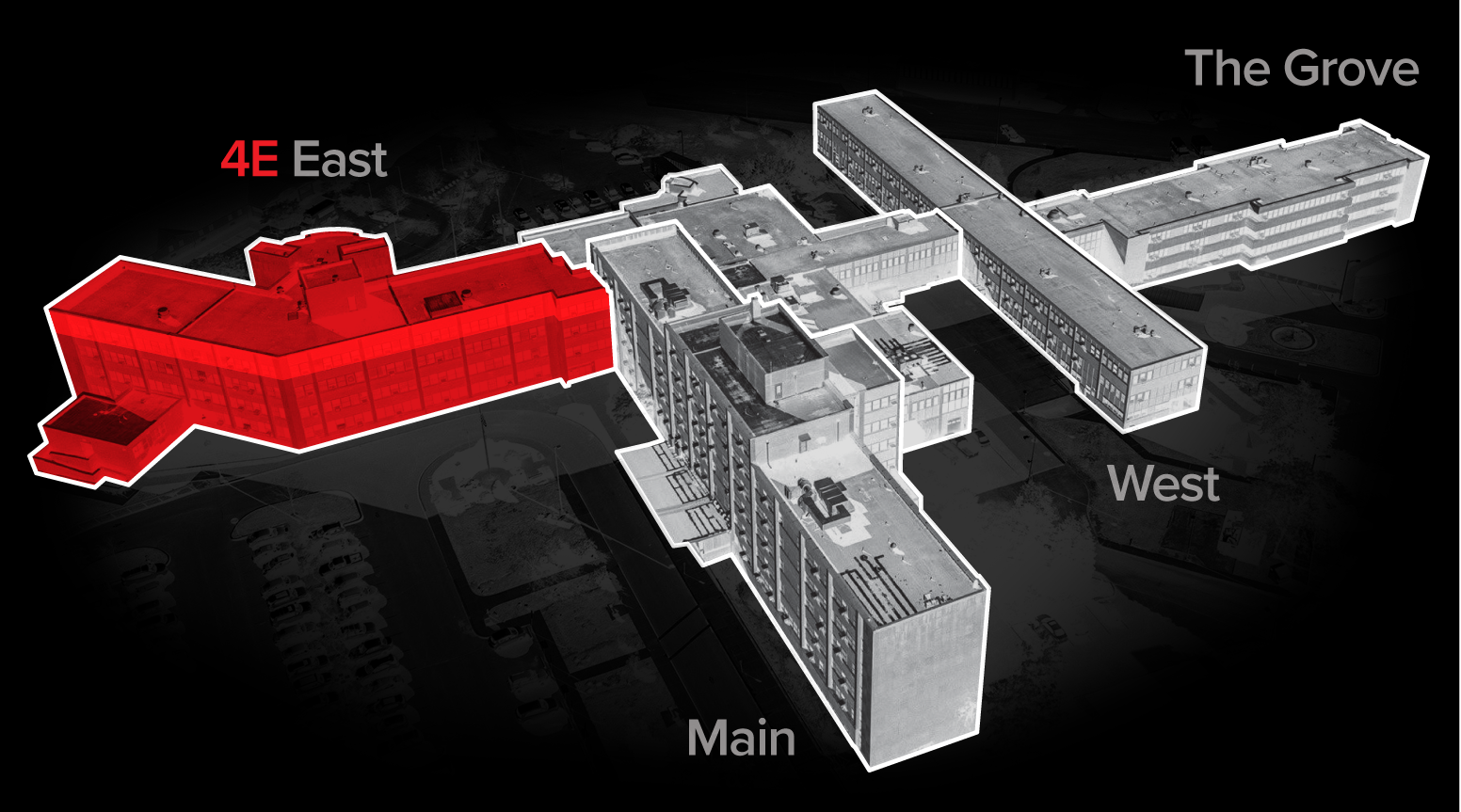
Mr. Denbow’s dementia unit on the 4th floor of the East wing was at the epicenter of the outbreak at Brighton, where three-quarters of the building’s then-460 residents — and 115 of its staff — eventually would test positive. Families and a resident said they believe at least half of the more than 50 residents in 4E died.
Brighton officials have refused to answer questions about deaths there.
“It was full before this started,” said John Bissell, a non-dementia resident of 4E who survived a COVID-19 infection and still lives there. “Too many of them died. Now there are only 26 people here.”
In a state with the fourth-highest nursing home population in the country, what happened at Brighton represents everything that went wrong with nursing homes during the deadly pandemic and illustrates why so many nursing home residents across the country like Mr. Denbow have died from the disease.
A five-month investigation by the Pittsburgh Post-Gazette found that the Beaver County nursing home’s owners, Comprehensive Healthcare, a for-profit company, and its managers failed to enforce even the most basic infection control standards during the worst of the outbreak.
In addition, decisions that Brighton’s owners made to significantly cut its full-time staff in the years after they bought the facility from Beaver County in 2014 played a critical role, as did a lack of training for new staff and poor communication among staffers.
All that may have set the stage for the deadly outbreak that is now the subject of two criminal investigations, one by the Pennsylvania Attorney General’s Office, the other by the FBI.
Brighton officials defended their actions, telling the Post-Gazette that by “early March” they had begun efforts to prevent COVID-19 from spreading, including screening visitors and staff.
But Ms. Boyer and more than a dozen other families who regularly visited loved ones there, as well as six staff members, say they never saw any such efforts before the center was locked down on March 12.
“Looking back now, that seems strange,” said Ms. Boyer, a school librarian who lives in Beaver Falls. “But at the time, it seemed everything was status quo, nothing had changed.”
Like more than 20 families the Post-Gazette spoke to during its investigation, Ms. Boyer, in the months after her father’s death, was left with troubling questions about what happened at Brighton and whether her father’s death could have been prevented.
Mr. Denbow, from Patterson, Beaver County, grew up in Coraopolis and served in the Army in Germany during the Vietnam War. When he returned from his service, he went to work in the same cement plant as his father, retiring in 2015 after 40 years there.
In retirement, he had grown particularly close to his grandchildren, A.J., 14, and Jonathan, 12. They were “the apple of his eye,” Ms. Boyer said, and were with her the last time she visited him.
Mr. Denbow, who had lived at Brighton for just over two years and suffered from Parkinson’s disease, began feeling ill the second week of March and was put on an IV. He tested positive for COVID-19 just two days before he died.
Family members of victims said they have been interviewed by attorneys from the attorney general’s office, and the FBI in September went to Brighton and another nursing home owned by Comprehensive Healthcare in Mt. Lebanon to execute search warrants for documents and data. Neither the FBI nor the attorney general would comment about the investigations.
Though nursing home residents represent just 5.7% of the 9.9 million positive cases recorded nationwide, they represent 38.6% of the 237,037 COVID-19 deaths as of Nov. 9. Those figures are even higher in Pennsylvania, where nursing home residents represent 6.5% of the state’s 238,657 positive cases and 42.3% of its 9,086 COVID-19 deaths.
Even among the many deadly nursing home outbreaks nationally and across the state, Brighton’s stands out — both in total numbers of cases and deaths, and in how pervasively the disease spread throughout the building among residents and staff.
Exactly who, or what, is to blame for Brighton’s outbreak is something family members have been thinking about for months. Most of the victims succumbed in the first six weeks of the outbreak, when, on average, nearly two residents a day were dying.
“There was a stretch there [in April] where, on a least a couple of days, we had three or four deaths a day,” said Tristan Adams, a former temporary “agency” nursing assistant who worked at Brighton for two years until July. “I didn’t have enough tears to cry anymore.”
A local funeral home operator, who asked not to be named, said he recalled one day in mid-April waiting to pick up the body of a resident: “I was in line with two other funeral home vans, all of us waiting for bodies. It was surreal.”
Ms. Boyer said figuring out what happened is important.
“I think that’s where I struggle,” she said. “Someone failed my dad, and I don’t know who to be angry with, whether it’s a system or a person. And I don’t know how to fix it, or who can fix it.”
In trying to find answers, the Post-Gazette interviewed residents, their family members, current and former employees, volunteers and nursing home experts. The newspaper also reviewed thousands of pages of state nursing home inspections and federal documents about the facility.
The PG found that efforts to cut costs led, in part, to the conditions that later allowed the coronavirus to flourish and spread. And after Brighton finally realized in late March that it had a deadly problem, it was slow to put in place and enforce the protocols that finally brought the virus under control, the investigation revealed.
Those findings are similar to some of the allegations in a lawsuit filed Oct. 21 by 15 families of those who died and residents who still live at Brighton. The complaint in that lawsuit alleges a direct causal connection between the conditions at the home and the deaths.
The PG’s investigation identified several missteps by the owner and its building managers:
The home failed to impose even basic infection-prevention protocols, such as limiting visitors, before the federal government told nursing homes to do so on March 12.
The private company significantly cut full-time, or its equivalent hours, in-house nursing staff after buying the nursing home from Beaver County in 2014.
It increasingly relied on part-time, often out-of-town, temporary “agency” nursing staff to care for residents, rather than using full-time, in-house staff.
It provided little or no training for nursing staff new to the building, and it did not properly communicate changes in infection-control procedures to all staffers.
The company in particular cut the overall staff hours of registered nurses, who are the most highly trained and most highly paid.
It moved some employees around the building shift-to-shift and sometimes during the same shift, potentially spreading the virus.
It housed most residents four to a room in the long-term care part of the building, when the current national and state nursing home standard is single or double occupancy.
After initially answering questions posed by the PG, Brighton officials in late September cut off correspondence, writing in an email: “Throughout the COVID-19 pandemic, Brighton has worked to closely follow the guidance of governmental health officials. Brighton is pleased to say the facility has now gone months without a new case of COVID-19. This is a testament to the dedication of our staff and the support of our residents and their families. Right now, the facility’s sole focus remains on ensuring the health and well-being of all residents and staff.”
That wasn’t the case in March, current and former employees said. There was a growing understanding of how deadly COVID-19 could be for the elderly and how nursing homes essentially were tinder boxes for the disease.
By the beginning of that month, said a former full-time Brighton employee, staff members were already talking about the Life Care Center in Kirkland, Wash., where 81 residents, 34 staff members and 14 visitors tested positive, with 37 of them dying.
“We saw what happened in the nursing home in Washington,” said the former employee, who left Brighton for a new job at the end of March and asked to remain anonymous. “And people [at Brighton] thought: What if that happens here?”
“But management didn’t think it would,” he said.
Next: A tale of two facilities
Sean D. Hamill
Daniel Marsula
Ed Yozwick
Andrew Rush
Laura Malt Schneiderman
Advertisement
Advertisement