That Facebook post led to calls from reporters. Dr. Thimons sounded prophetic when he told WPXI-TV on March 18, “We don’t know what to do. Right now we’re … sending patients back to nursing homes with suspected coronavirus where they could infect 100 other people there, where mortality rates in nursing homes may be 10 to 20%. We’re looking at massive amounts of deaths and a huge tragedy.”
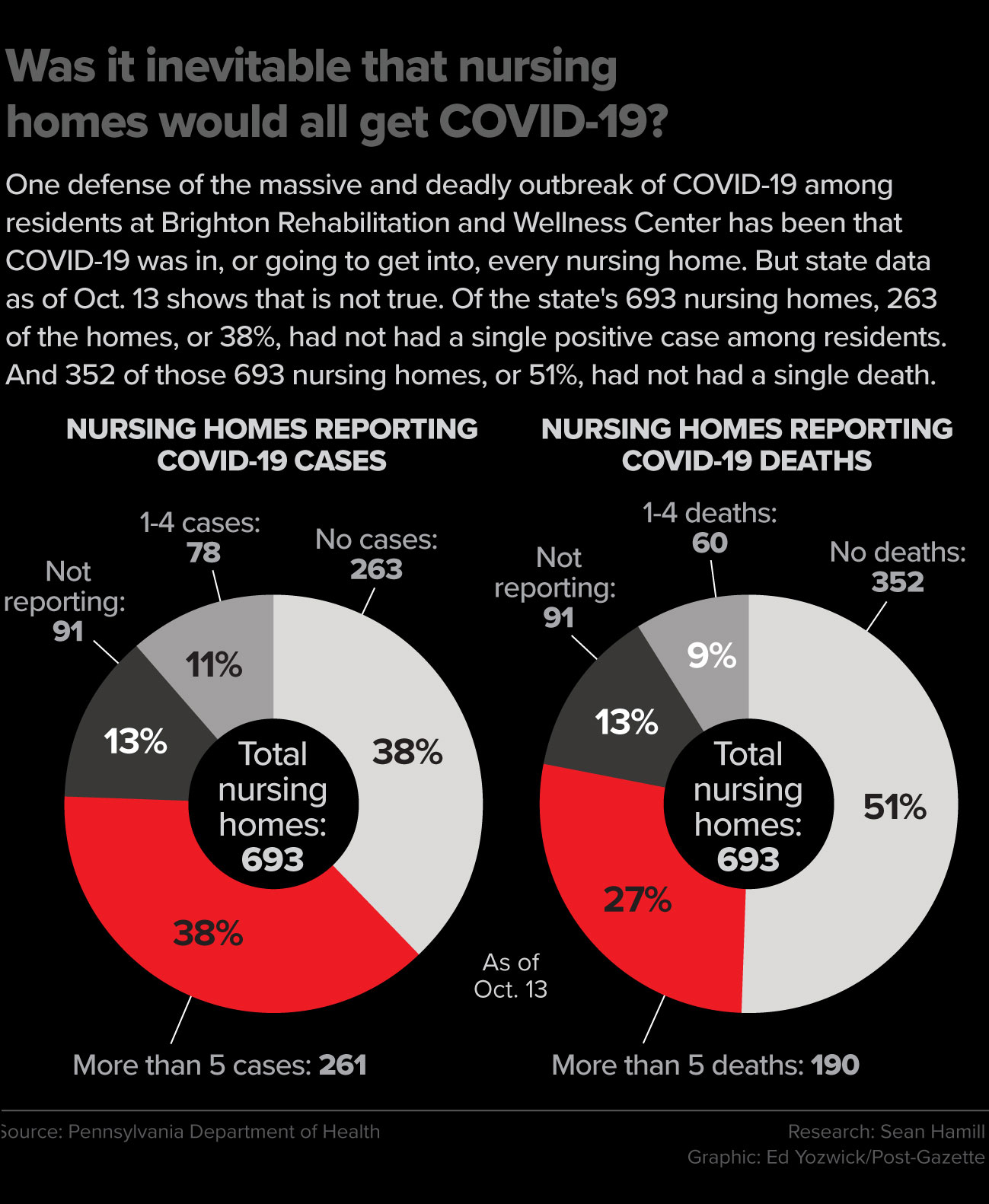
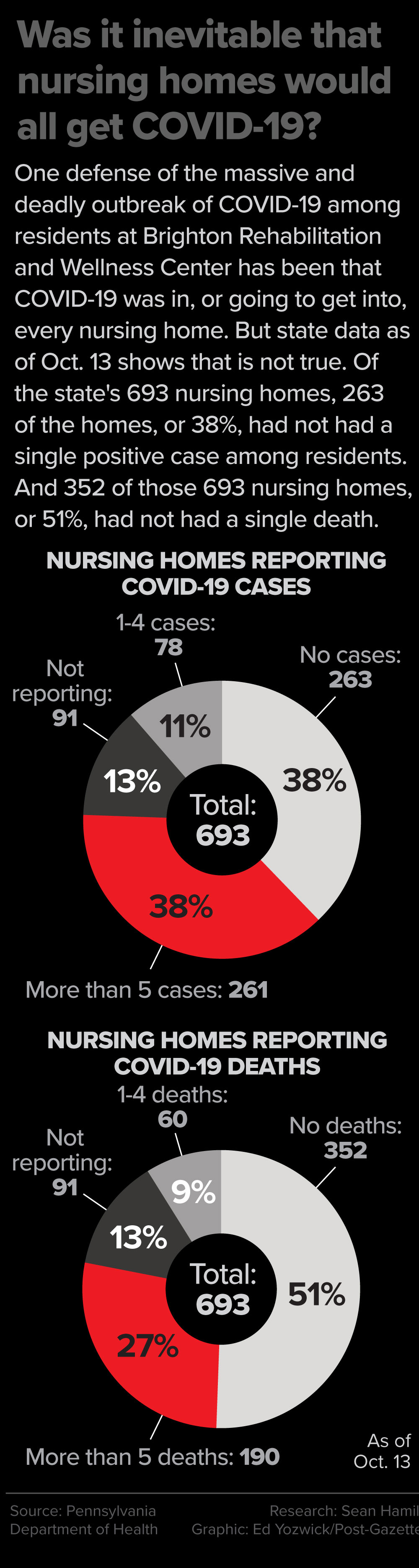
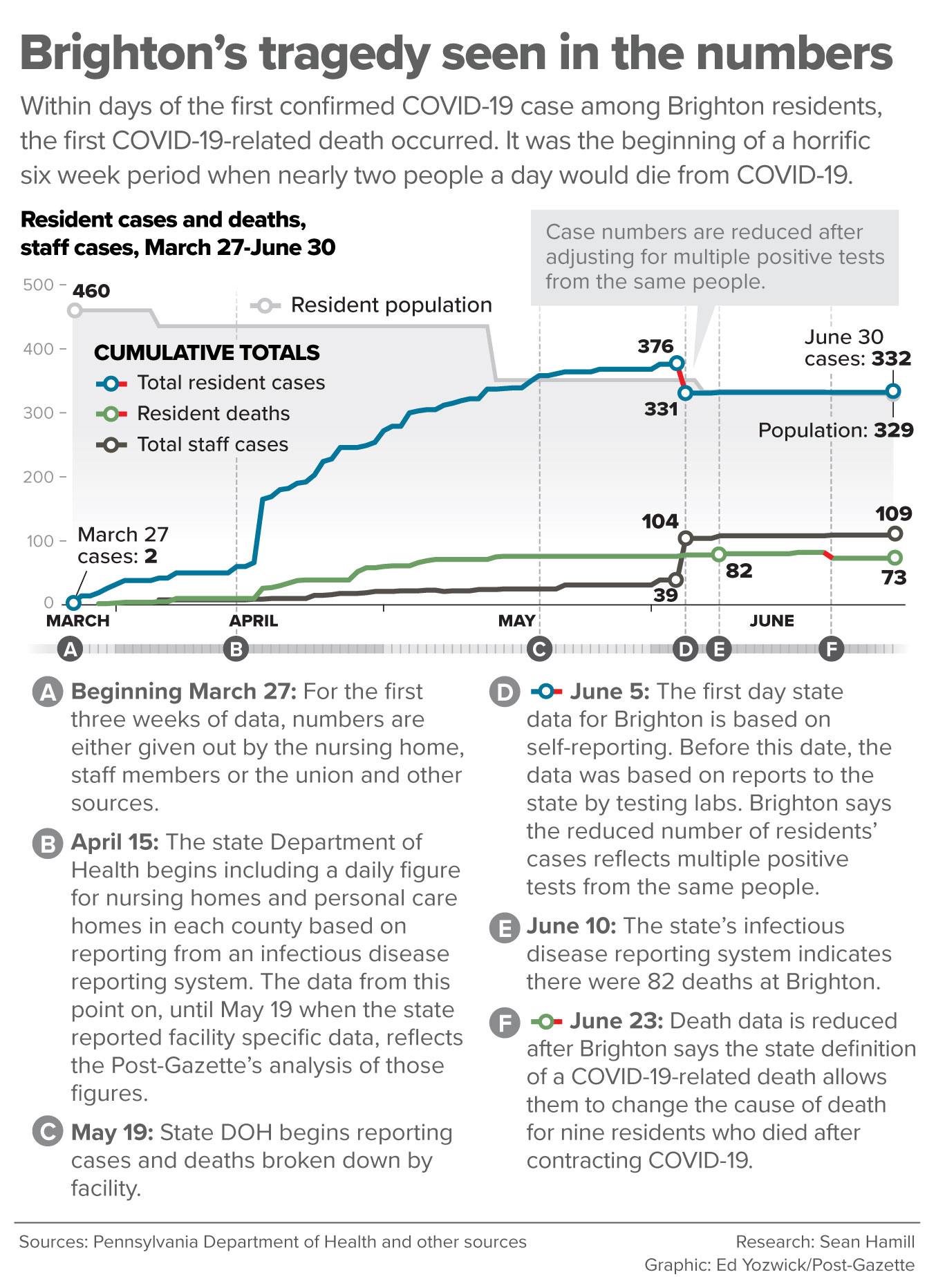
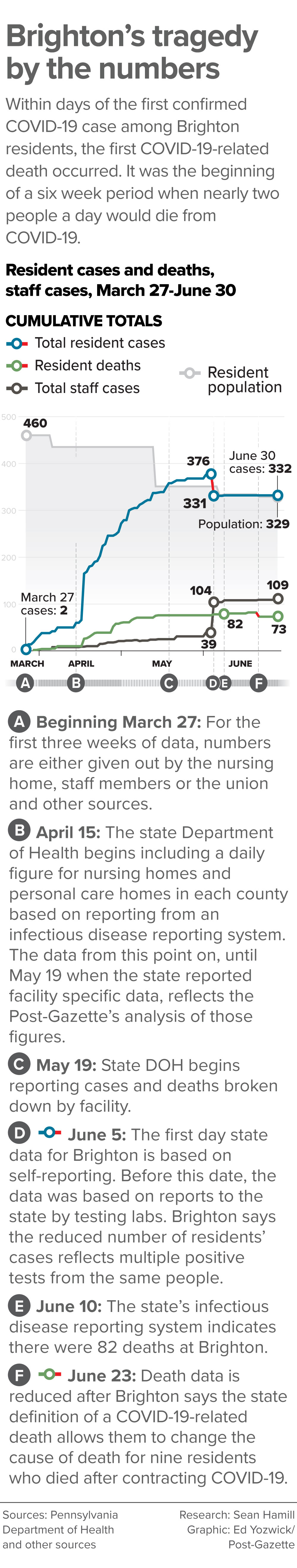
Dr. Thimons’ prediction would prove to be an underestimate for Brighton: The mortality rate there — at least 82 residents eventually dying from among the 332 who tested positive — was 25%.
Brighton says by its own count, only 73 residents have died from COVID-19. In late June, it removed nine residents from its self-reported data given to the state each week.
To do that, Brighton used a disputed state definition of who could be classified as a COVID-19-related death.
The state definition allowed nursing homes not to count someone who died after contracting COVID-19 if they had met criteria for having “recovered” before they died.
The state said that was based on the federal Centers for Disease Control and Prevention’s definition of recovered. But the CDC said the designation was not intended to to be applied to COVID-19-related deaths, just to whether a person with the disease could be removed from isolation.
Brighton’s actual COVID-19 death count may be even higher than 82. Three families told the Post-Gazette they had loved ones die of what was listed as “pneumonia” on their death certificates. The families said their relatives were never tested for COVID-19, even though they had symptoms and others who lived in their rooms or unit had tested positive.
Three more families said the deaths of their relatives, who also had symptoms or were in rooms where others tested positive, were recorded as “dementia” or “Alzheimer’s.”
Those six residents could have died from the causes listed on the death certificates, but all of the families said they were told that the victims had symptoms similar to COVID-19 — such as a fever or shortness of breath — but were not tested.
It is unclear exactly how many people have died without being tested, and Brighton would not provide a figure when asked.
Brighton reported its population at the beginning of April as 460, and the state said Brighton voluntarily stopped taking new residents in early April. By the time the state declared June 10 that 82 people had died, Brighton said the building’s population was just 334 — 126 fewer in just 10 weeks. That means 44 other residents either died or left the building during that time.
Families say they were told that as many as 20 residents were moved out as the outbreak swept through the buildings.
But exactly how many of those 44 residents were moved, died of COVID-19 or died from some other cause could not be determined. Brighton would not provide a breakdown when the Post-Gazette asked specifically for that information.
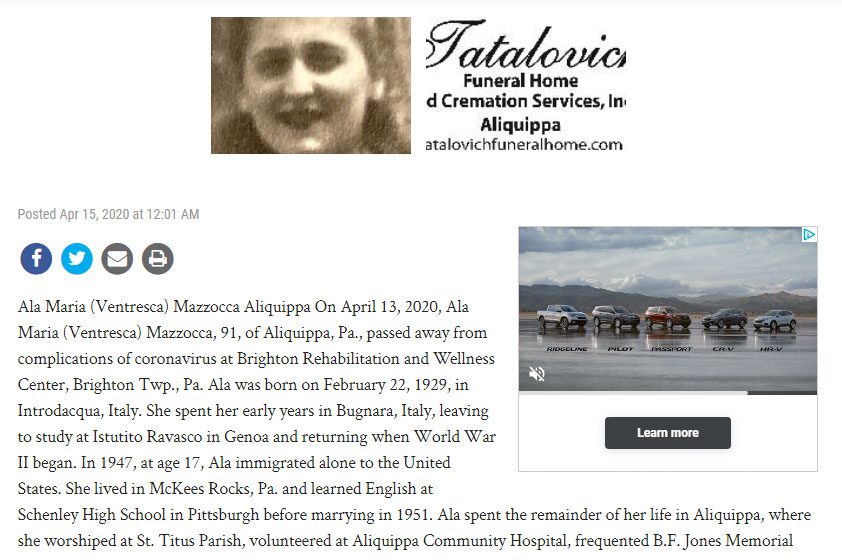
Ala Mazzocca, 91, a five-year resident of Brighton originally from Aliquippa, was one of those who died but was not tested.
On April 8, nurses said Mrs. Mazzocca had bedsores — a problem Brighton had been cited for in the past and that nursing home experts say is a sign of an overwhelmed staff that could not attend to her properly — and her dementia was worsening. Five days later, a staff member called to say that she had died of “respiratory distress” overnight on April 13. On her death certificate, signed by Dr. Laura Mantine, a physician working for Dr. Thimons’ practice, the cause was listed as pneumonia.
It was a stunning conclusion, said her grandson, Andrew Macurak of Washington, D.C. The family had not heard of any respiratory issues before that. “You don’t suddenly get pneumonia overnight,” he said.
The family said in her obituary that she was a victim of the coronavirus.
“It was obvious what she died of,” Mr. Macurak said.
Next: “Everyone’s sick.”