Jacob Albertson and his sister Bernadette Brenkus visit their mother Debra Albertson, a resident of Brighton Rehabilitation and Wellness Center. (Andrew Rush/Post-Gazette)
An increase in rehabilitation
Before the 2014 sale, the county received about $1 million a year from Medicare for providing physical, occupational and speech therapy.
Comprehensive drove that revenue to more than $9.5 million by 2018. It came from Medicare, Medicaid and private pay sources, with $8.6 million coming from Medicare alone in rehabilitation fees.
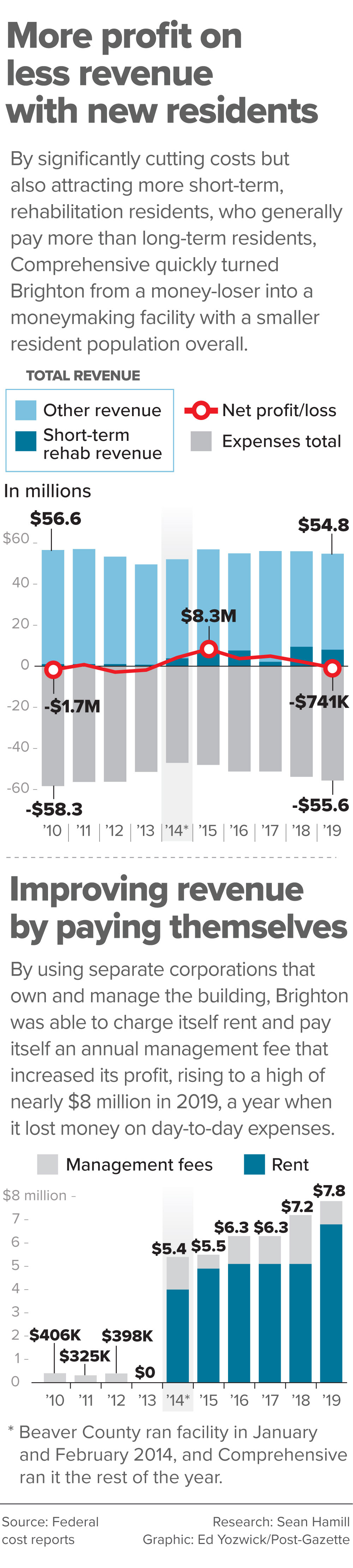
That increase in rehabilitation revenue helped push Comprehensive’s annual profits at Brighton up immediately. It made $4.1 million its first year, 2014, doubling that in 2015, to $8.2 million, and it made at least $2.2 million each year until 2019, when an increase in nursing staff expenses resulted in its first loss — $741,000 — since it bought the nursing home.
Comprehensive has found other ways to make money off of Brighton, too. Each year, one Comprehensive corporation that manages the building pays rent to another Comprehensive corporation that owns the building — rent that has steadily risen from $3.9 million in 2014 to $6.8 million in 2019. In addition, Comprehensive pays itself a “management fee” that has averaged $1.2 million a year.
The state Department of Human Services says both payment methods are legal under nursing home regulations.
But critics say that allowing nursing homes to charge themselves rent and management fees is a way to appear to have lower profits than they actually do, which not only potentially reduces their tax liability, it allows nursing homes to argue for more funding.
“It’s a shell game,” said Brian Lee, former long-term care ombudsman for Florida and now executive director of the nursing home resident advocacy group Families for Better Care. “It dupes the state officials into thinking [nursing homes] have razor thin margins.”